The real voyage of discovery consists not in seeking new landscapes, but in having new eyes. – Marcel Proust
We kicked off 2022 with this series we’re wrapping up today: Transforming primary care encounters by taking a solution-focused approach when managing type 2 diabetes in the primary care setting. Along the way we’ve shared a multitude of tips and tactics to add to your toolbox so speak. Today’s blog wraps up the series as we focus on discovery learning from diabetes data in a solution-focused way.
While there is a multitude of diabetes data that we can learn from, today we’re focusing on structured blood glucose monitoring (BGM) and professional continuous glucose monitoring (CGM).
DISCOVERY LEARNING FROM STRUCTURED BGM
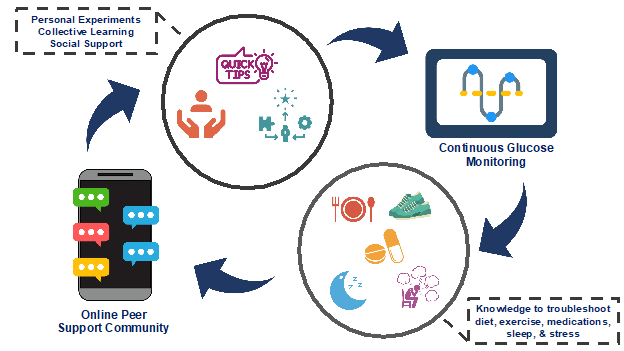
Both of us spent a large portion of our career in the primary care setting where we routinely used structured BGM.There are 3 profiles that we have routinely used with clients/patients to help them to discover and learn about their blood glucose patterns and how favorite foods and physical activity affect them. We call this “discovery learning” because on their own, using “personal experiments” people are uncovering aspects of their diabetes themselves. And when people learn by doing, they are able to make health decisions that work for them. They are identifying “what’s working well” and are able to apply solution focused tactics to “do more of what’s working” and focus on successes instead of problems. Discovery learning is a great way to incorporate a solution-focused approach into practice. Let’s look at some examples
When using BGM there are several profiles or checking patterns you can apply.
7-point profile
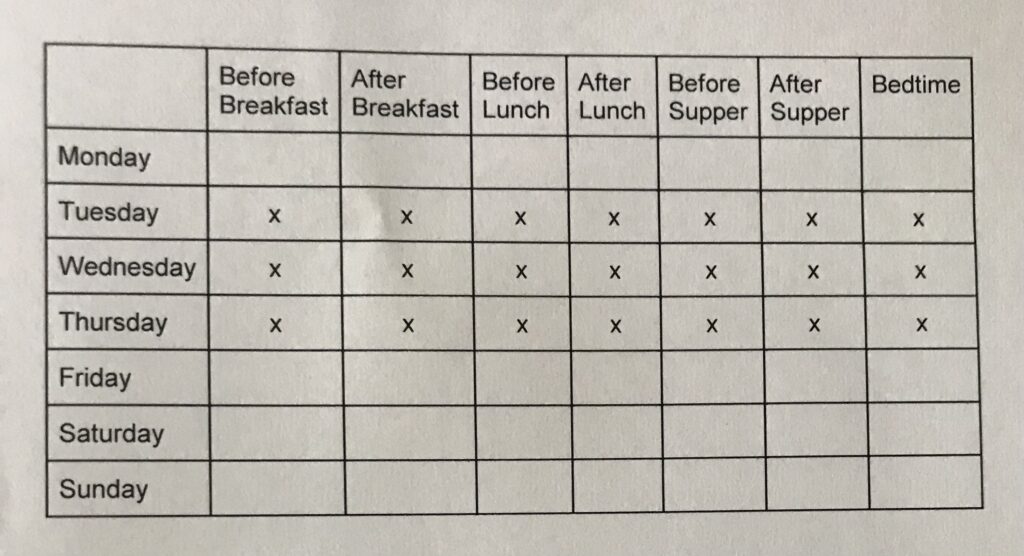
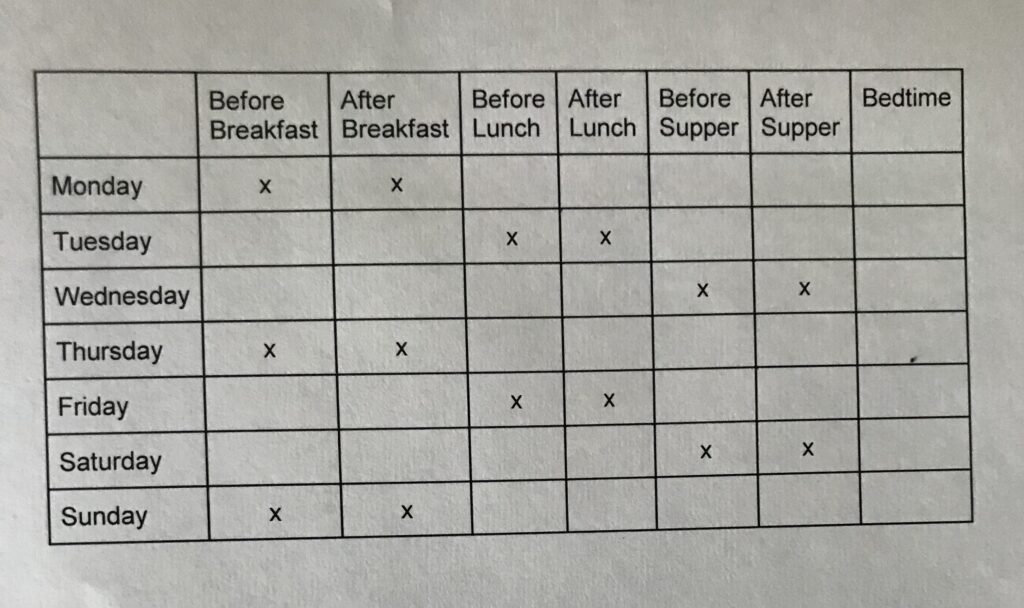
This one can be helpful to use for 3 days prior to a visit, for instance. This profile uses 21 strips, or 7 checks (before and after each meal and at bedtime) 3 days in a row. See the table below. The concentrated focus helps to measure the magnitude and frequency of short term fluctuation in blood glucose. It can be helpful in reducing the therapeutic inertia (Read more about therapeutic inertia in our blog here.)
5-point profile
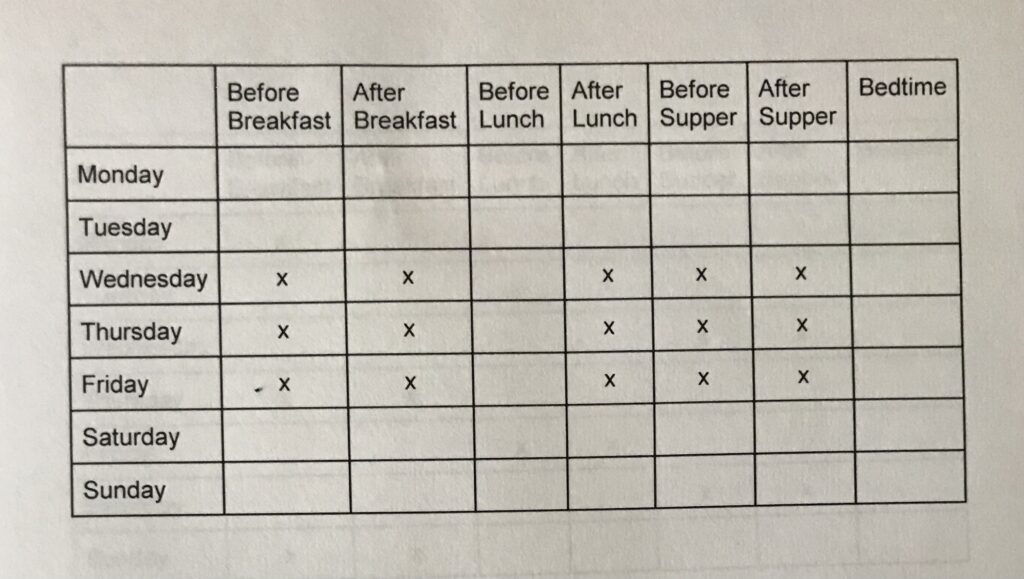
Similarly is the 5-point profile which requires fewer strips (15), if supply of adequate test strips is a concern. The 5-point profile includes 5 checks daily for 3 days, as you see in the table below – checking before and after breakfast and supper, as well as after lunch.
Paired checking
This is one of our favorite profiles for discovery learning. It can be used to focus on one thing, such as how a food/meal impacts blood glucose. We’ve had many clients/patients use paired checking to learn how their Friday night pizza affects their blood glucose. One example that stands out was an individual who routinely ate ½ of a medium hand-tossed pepperoni pizza (4 slices). After seeing the spike in his blood glucose, he decided to go with 2 slices and a side green salad, and saw his blood glucose fall back into range. We encourage patients to conduct their own “experiments”, if you will, to learn how food (type, portion) or adding in more physical activity affects them.
Paired checking can also be used around 1 meal time each day, rotating amongst the meals over the course of the week, to give a good look at blood glucose patterns.
Follow-up on personal experiments
At the follow-up to see what the individual learned from structured BGM, ask solution-focused questions in a non-judgemental way, such as:
I know you really like cheesecake and were planning to try paired checking to see how 3 bites satisfied you and affected your blood glucose, as compared to eating a whole piece. What did you learn? Did that change your plans? What are some options if your glucose spikes?
What have you learned during your discovery? And follow up with, How can you do more of that?
DISCOVERY LEARNING FROM PROFESSIONAL CGM
Another tool available to support people with type 2 diabetes to engage in discovery learning is by using professional CGM. Professional CGM is owned by the clinic, not the person with diabetes, for intermittent CGM use. Similar to the personal experiments described with BGM, a person can choose to view their data before and after favorite foods, different activities, or even before and after sleep or a stressful event. The benefit of professional CGM is that the individual doesn’t have to do a fingerstick as the unblinded professional CGM can be connected to their smartphone and they are able to see their data in real time for up to 10 days. We’ve written about discovery learning and CGM previously. There is also a blinded professional CGM where the person reviews the data at the end of session retrospectively. While not as useful for discovery learning and personal experiments, if they keep good records of food and activity they can identify trends and patterns.
Examples of personal experiments:
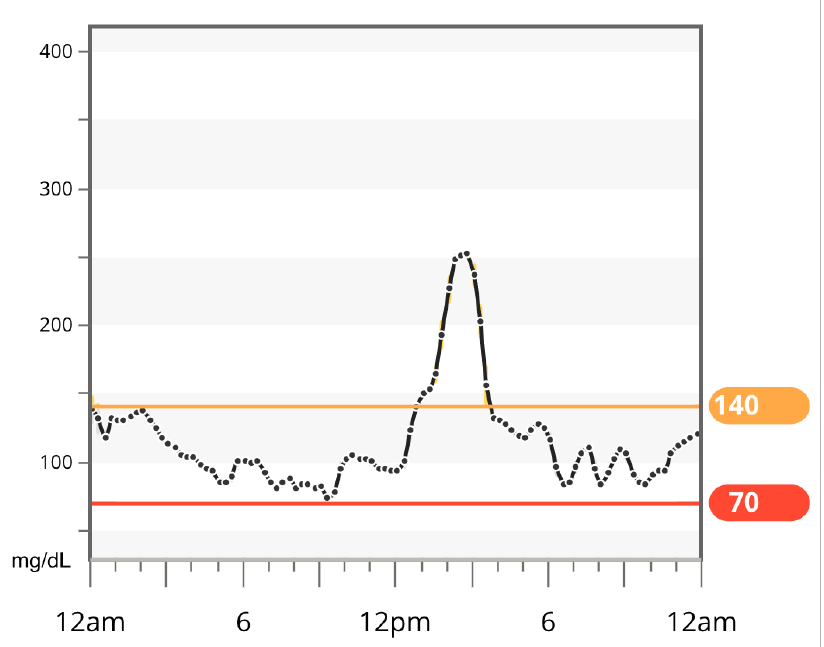
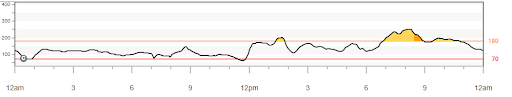
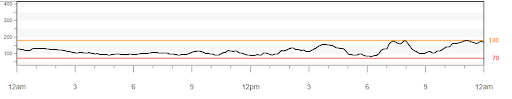
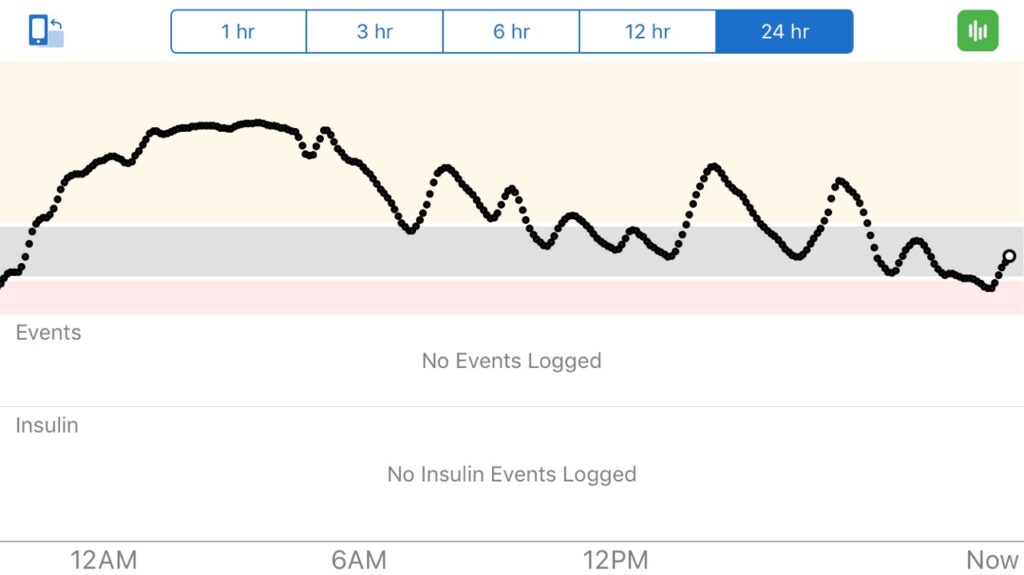
Favorite foods – While wearing the CGM your client might decide to eat different breakfasts each day of the week, and view their data on their smartphone before and again two hours later to see if they stayed in their target range (typically 70mg/dL-180mg/dL). They might choose their favorite high carb breakfast one day, and then a low carb version the second day, and then something in-between the next day.The beauty of personal experiments is that they can be anything that matters to the person.Through this personal discovery, they are able to learn what is working and make decisions.regarding their next steps.
Physical activity – Similar to evaluating the impact of food on glucose values, the same can be done for physical activity. The client can check their smartphone to know their glucose value and their trend arrow direction (are they staying steady, trending up or down) and then choose a variety of physical activities to evaluate the impact. Some questions they may ask are: What happens when I start physical activity when I have a trend arrow going down but my glucose is in range? Or what happens when I complete my physical activity and my trend arrow is going up? Many people discover that their glucose values actually increase following physical activity, but then come down later and using CGM can help them to plan how they respond.
Stress – Using CGM can really help clients understand the impact stress can have on their glucose. We’ve shared in our presentations about a friend who’s CGM values went straight up during a stressful event when she had nothing to eat or drink (the fire alarm went off, she ran out of her condo but forgot to get her cat …good news in the end it was a false alarm and the cat was fine!). Viewing data during stressful times can help people remove some of the guilt they experience with glucose fluctuations and help them to realize that diabetes is a challenging condition to manage.
Follow-up on personal experiments
Similar to BGM, use your solution-focused tools when discussing data. Focus on what went well, what the individual learned, and remember that all data are valuable. Data are just numbers and not judgements and do not define a person as “good” or “bad.” Help your clients value data to support their learning and to modify their health behaviors, even when their choices may not be choices you would suggest. People need to be ready to make big changes, and over time, data can help them get there!
I see you changed how much you walked after dinner, what did you learn?
You were in target range after these three meals, how did you do that? How can you do more of that? And what else?
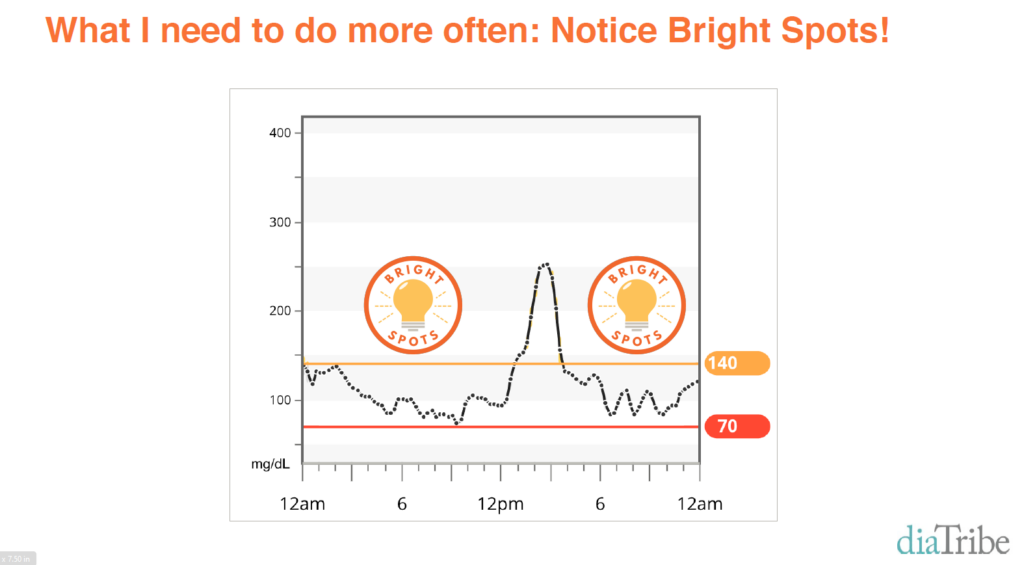
We’ve written before about the 42 different factors that affect glucose (see Bright Spots and Landmines) and how Bright Spots are very similar to “exceptions” in a solution-focused approach, a time when things are going well. Author Adam Brown mentions that he would not have been able to identify these 42 factors without the use of CGM to guide him and reveal glucose changes that were unknown before. There is nothing more helpful for someone trying to make a challenging health behavior change than personal data to help them identify what they can do and what is reasonable for them.
Stop back by in 2 weeks when we’ll share a sneak peek at our session we’ll be presenting at the ADCES22 conference in Baltimore, MD!
We welcome anyone interested in our approach to Subscribe to our blog and we’ll email you when a new post is published!
If you are a health care professional and interested in learning more about our solution-focused practice and approach, when you subscribe to our blog, we’ll send you in return a FREE resource of 10 Solution-Focused Questions to start a solution-focused discussion with your clients.
Follow us on Twitter and Instagram @AFreshPOVforYou
Deb is employed by Dexcom, but her words and opinions in this blog are her own.
Tami is employed by the University of Kentucky HealthCare Barnstable Brown Diabetes Center, but her words and opinions in this blog are her own.